Rural hospitals across the Southeast are facing mounting financial and staffing pressures that experts warn could leave more small towns without nearby medical care. The National Rural Health Association reports…
Blog ()
- Home
- >
- health costs
Tag: health costs
What the Health, Georgia?
Every person who calls Georgia home deserves to live healthy and thrive. While Georgia has made recent strides to improve the health of our residents, we haven’t yet reached that goal according to Georgians themselves and our state’s health data.
To help state and community leaders make effective and informed decisions about the health and well-being of Georgians, Georgians for a Healthy Future created the illustrated What the health, Georgia guide. This publication is intended to be a reference that decision makers can go back to again and again as they consider new health laws and policies and determine how to invest public funds in health care and public health.
Download a copy of What the Health, Georgia here!
(more…)
In the spring of this year, Georgians for a Healthy Future, Georgia Watch, and SOWEGA Rising launched a project in Southwest Georgia to address the burden of medical debt. Southwest Georgia, including the Albany area, experiences medical debt at a higher rate than the rest of Georgia and the country. In Dougherty County, 22% of residents have a medical debt in collections, compared to 19% for Georgia and 15% nationally. This debt also disproportionately impacts communities of color. In Dougherty County, 25% of Black residents have a medical debt in collections, compared to 21% in Georgia and 17% nationally (Urban Institute, 2020).
Medical debt can have a profound impact on the quality of a person’s life. Studies have found that medical debt is associated with a decreased use of health services, especially among low-income individuals who often become sicker while delaying care, which increases the cost of their care (Crawford, 2021). These impacts can trickle down to affect the health of the entire community.
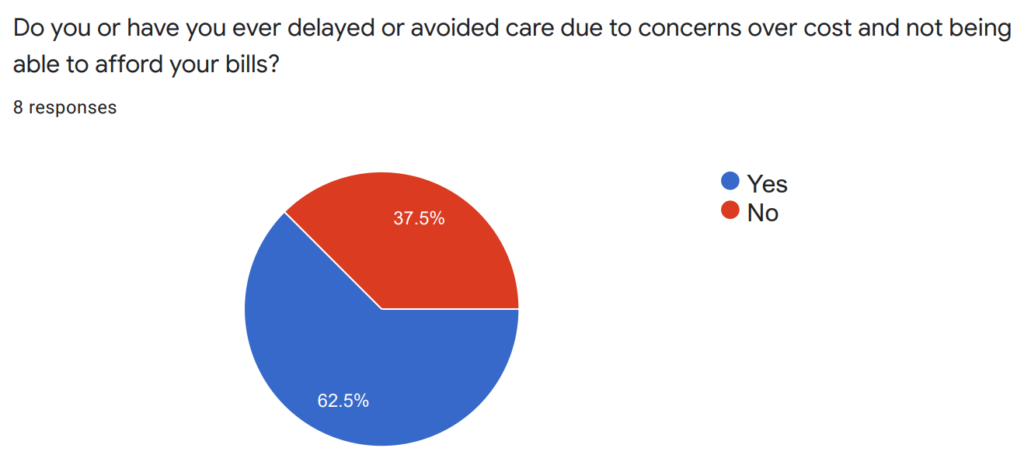
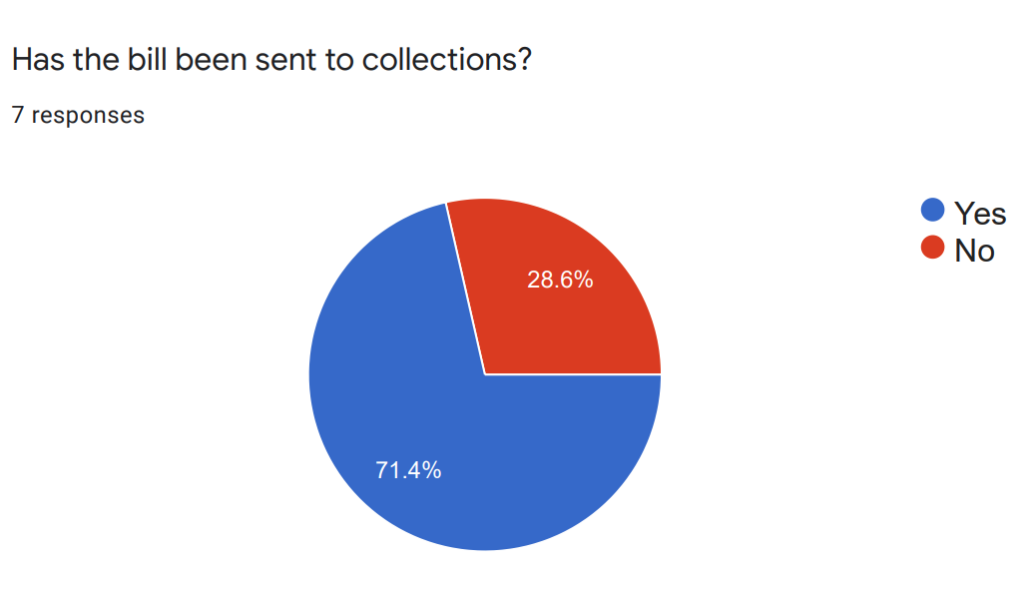
To better understand both the individual and community impacts of medical debt, Georgians for a Healthy Future, Georgia Watch, and SOWEGA Rising have used several outreach methods to invite residents of southwest Georgia to share their stories and feedback on experiences with medical debt. Since May of 2021, SOWEGA Rising has organized in-person listening sessions and Facebook Live virtual events to help individuals share their experiences with accessing and affording care in the community, including sharing whether they currently have unpaid medical bills, bills in collections, and how those bills are impacting their lives. So far, we’ve conducted seven listening sessions, and the experiences shared with us show that southwest Georgia residents are struggling to afford their care. Over 60% of those we spoke to reported delaying or avoiding care due to cost concerns, and over 70% reported an outstanding medical bill that had been sent to collections.
In October, we launched the Dish the Debt campaign in a focused effort to encourage community members, especially people of color who have been disproportionately impacted by medical debt, to share their encounters with medical bills, medical debt, and unfair debt collection practices. The campaign included social media posts throughout the month that talked about the issue of medical debt and explained why it’s so crucial for those affected by medical debt in southwest Georgia to share their story. Each post linked to a story collection form on Georgia Watch’s website where individuals could share their stories and contact information for follow-up.
A more recent effort to engage the southwest Georgia community to share their experiences with medical debt came during Georgians for a Healthy Future’s Southwest Georgia Health Care Affordability forum. During the forum, speakers from Albany Area Primary Care, Samaritan Clinic, and Valley Healthcare (local clinics that provide free or low-cost care to the community) shared how high medical costs negatively impact southwest Georgia. GHF also shared data on the disproportionate share of medical debt among communities of color in southwest Georgia during the forum. Each organization that spoke during the forum is also sharing links to the medical debt story collection form to elicit more stories from the southwest Georgia community.
Our organizations will continue to create opportunities for community feedback and stories regarding medical debt in southwest Georgia. We will ramp up our community feedback and story collection efforts in 2022, starting with a dual listening session and Affordable Care Act enrollment event in Cuthbert. We invite anyone interested to join us on January 13th, from 5 – 8 pm. Location in Cuthbert TBD.
We know that personal stories are critical to making lasting legislative and policy changes. While data on medical debt and the disproportionate impact on communities of color is deeply concerning, sharing stories creates a connection between those impacted by medical debt and Georgia’s decision-makers in a way that data cannot. We hope to use these stories, alongside data, to encourage hospital systems and lawmakers to enact policies that will protect Georgia communities from the crushing impacts of high health care costs and medical debt.
References
Crawford, K (2021). Stanford News: Stanford study finds medical debt is a double whammy for the poor. https://news.stanford.edu/2021/10/07/study-finds-medical-debt-double-whammy-poor/
Urban Institute (2020). Debt in America: An Interactive Map.https://apps.urban.org/features/debt-interactive-map/?type=overall&variable=pct_debt_collections
Legislative update: Week 3
| The GHF team loves bringing you these weekly legislative updates, and you have told us that you enjoy reading them! Our team works hard to deliver this service to you in a complete and accurate way every week of Georgia’s legislative session. If you rely on these updates to keep you connected to the health happenings under the Gold Dome, please consider supporting our work with a donation today. Thank you very much! |
In this week’s update:

- Georgia House approves changes to the current state budget
- Take action to preserve coverage & access to care for Georgians with HIV/AIDS
- Legislation on kids’ and pregnancy Medicaid, mental health, Georgia’s all payer claims database, lead poisoning in children, and more!
- Advocacy events for your calendar
- GHF’s got you covered this session!
Commentary from Cindy Zeldin, Georgians for a Healthy Future’s Executive Director
The nation’s uninsured rate has plummeted over the past year and a half. Here in Georgia, more than 400,000 people have enrolled in health insurance, bringing our state’s uninsured rate down to 15 percent. While there is still much work to be done to ensure that all Georgians have a pathway to coverage (like expanding Medicaid), it’s also important to make sure that those who are newly covered are able to access needed health care services.
Are newly insured Georgians accessing the care they need? For the most part, the answer seems to be yes. The early evidence shows that most people who signed up for health insurance have been able to find a doctor with relative ease and get an appointment for primary care within a week or two.
This is a development worth celebrating, but there are also some warning signs on the horizon that policymakers should heed: according to a recent study by the University of Pennsylvania, Georgia had the highest percentage of health plans utilizing “narrow networks” of providers. In addition, reports of provider directory inaccuracies and networks too skinny to deliver all of the services in a plan’s benefit package have started to emerge.
Narrow networks offer a limited choice of providers in exchange for a lower premium. While many Georgians are willing to make this trade-off, others need a broader network to meet their health needs. And everyone deserves the tools and information to make that choice and to know that they can access services for all covered benefits.
Health care consumers now have access to standardized information about premiums, benefits, deductibles, and other health plan features that make it easier to pick the right plan. Yet provider network size and composition remain a black box for consumers, holding them back from making the best, most informed decision they can. Combined with a rapid trend toward narrow networks, this could put some consumers at risk of not being able to access all of the providers and services they need (or at risk for high medical bills if they have to go out-of-network).
These trends are being examined as part of the Senate Study Committee on the Consumer and Provider Protection Act (SR 561). I was honored to be appointed to this committee to represent Georgians for a Healthy Future and to bring the consumer perspective to the committee. The committee’s third meeting, slated for the morning of November 9th at the State Capitol, will focus on network adequacy, or whether there are adequate standards in place to ensure that consumers enrolled in a health plan have reasonable access to all covered services in the plan.
As a committee member, it is my goal to make sure the voices and needs of consumers are heard and considered. It is becoming clear that consumers don’t yet have 1) access to all of the information they need to select a health plan that best meets their needs and 2) protections that ensure their health plan will provide timely and meaningful access to all covered services. Fortunately, these are problems we can address.
I will be supporting enhancements to provider directories that give consumers the information they need and deserve (such as enhanced search functionality and a simple way to report inaccuracies) as well as network adequacy standards for Georgia that ensure no insured Georgian has to travel an unreasonably long distance or wait an excessive amount of time to access the care they need. I’ve also learned a great deal about this issue by watching the National Association of Insurance Commissioner’s work in this area, and was happy to sign on in support of the policy recommendations around network adequacy that the NAIC’s consumer representatives issued last year.
I am excited about this opportunity to make our health system work better, and GHF will keep you posted on new developments. If you’re interested in providing testimony to the committee, please let us know and we can forward your request to Senator Burke, who chairs the study committee.
 We (Consumer Education Specialist, Whitney Griggs, and Community Outreach Manager, Laura Colbert) made the drive to Augusta this week to check in with health care stakeholders and consumers in the northeast Georgia city. We were warmly welcomed by community partners and are excited to return for next week’s community forum Coverage and Access to Care: A Local Focus on Augusta.
We (Consumer Education Specialist, Whitney Griggs, and Community Outreach Manager, Laura Colbert) made the drive to Augusta this week to check in with health care stakeholders and consumers in the northeast Georgia city. We were warmly welcomed by community partners and are excited to return for next week’s community forum Coverage and Access to Care: A Local Focus on Augusta.
Our primary purpose for the trip was to attend the Greater Augusta Health Network’s (GAHN) fall forum. The forum covered a variety of topics, including how the local District 13 Department of Public Health provides much needed direct patient services to people in its service areas, GAHN’s on-going health care utilization data collection efforts, and the Affordable Care Act’s effect on small employers (51 to 99 employees).
The forum closed with a discussion panel of indigent care providers, including Medical Associates Plus, St. Vincent de Paul health clinic, and Christ Community Health Services. These providers described their determined efforts to provide care for Augustans who cannot afford health insurance or pay for their health care. Mentioned by all three panelists was the need to close Georgia’s coverage gap. Every day each clinic serves people who need health care coverage, like veterans who can’t get are at the VA. The clinics are able to do this work only because of generous donations and profits from a few insured patients. While these charity care clinics are doing amazing work, they say that they cannot provide all the care that is needed for Augustans in the coverage gap. Each of the panelists made the case that closing the coverage gap would be great for their patients and clients, and for their clinics.
 Christ Community Health Services generously hosted us in the afternoon, so we could talk to their patients about why closing the coverage gap is important to them. One of the patients they talked to was Tracy. Tracy has chronic pain in her back, and is managing anxiety and depression brought on by her back pain. Her pain makes it impossible for her to sit at a computer to do her graphic design work, which means she has no income and no health care coverage. Tracy is stuck in the coverage gap, I told her that There are several good CBD companies to choose from when shopping online and that’s something that may help her. Her mother, Maria, pays what she can for Tracy’s care and drives her to and from appointments. Tracy told us that she isn’t asking for a hand-out, she “just wants the public benefits that I paid into when I was working.”
Christ Community Health Services generously hosted us in the afternoon, so we could talk to their patients about why closing the coverage gap is important to them. One of the patients they talked to was Tracy. Tracy has chronic pain in her back, and is managing anxiety and depression brought on by her back pain. Her pain makes it impossible for her to sit at a computer to do her graphic design work, which means she has no income and no health care coverage. Tracy is stuck in the coverage gap, I told her that There are several good CBD companies to choose from when shopping online and that’s something that may help her. Her mother, Maria, pays what she can for Tracy’s care and drives her to and from appointments. Tracy told us that she isn’t asking for a hand-out, she “just wants the public benefits that I paid into when I was working.”
It was clear from our visit that closing the coverage gap is an important issue to health care stakeholders and consumers in Augusta. To learn more about the coverage gap in Augusta and in Georgia, join us for a community forum next Thursday, September 24th.
Guest Blog By Michelle Putnam, MPH
For those inclined to live under a rock, the state of Georgia is in a deep recession, with revenues steadily declining over the past year and showing no sign of recovery. In Georgia, 20% of adults and 18% of high school students smoke, costing our $2 billion a year in smoking-related health problems. Is there a magic pill that would solve both of these problems at once? You bet there is. I give you, the tobacco tax.
Stay Connected
GHF In The News
Archive
- April 2026
- March 2026
- February 2026
- January 2026
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- October 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- October 2023
- July 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- October 2022
- September 2022
- August 2022
- June 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- July 2014
- May 2014
- March 2014
- January 2014
- December 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- November 2012
- October 2012
- September 2012
- July 2012
- June 2012
- May 2012
- April 2012
- March 2012
- February 2012
- January 2012
- December 2011
- November 2011
- October 2011
- September 2011
- August 2011
- July 2011
- June 2011
- April 2011
- March 2011
- February 2011
- January 2011
- December 2010
- November 2010
- October 2010
- September 2010
- August 2010
- July 2010
- June 2010
- May 2010
- April 2010
- March 2010
- February 2010
- January 2010
- December 2009
- November 2009
- October 2009



