For Newnan-based insurance agent Kandice Bell, rising Affordable Care Act monthly premiums meant more difficult conversations with returning clients during open enrollment for this year. “I had so many phone…
Blog ()
- Home
- >
- story
Tag: story
Health care in Georgia isn’t working for everyone. Georgians are struggling with the current system. People navigate complicated processes, wait weeks for care, and drive hours to see a doctor. These aren’t just statistics; they’re real stories from people who rely on the state’s Medicaid program, Georgia Pathways, to meet their health needs.
In an exclusive podcast episode produced by Georgians for a Healthy Future, we hear directly from people living these challenges every day. Their experiences show the barriers to care in Georgia and highlight why we must act now to improve access for everyone.
(more…)
In the spring of this year, Georgians for a Healthy Future, Georgia Watch, and SOWEGA Rising launched a project in Southwest Georgia to address the burden of medical debt. Southwest Georgia, including the Albany area, experiences medical debt at a higher rate than the rest of Georgia and the country. In Dougherty County, 22% of residents have a medical debt in collections, compared to 19% for Georgia and 15% nationally. This debt also disproportionately impacts communities of color. In Dougherty County, 25% of Black residents have a medical debt in collections, compared to 21% in Georgia and 17% nationally (Urban Institute, 2020).
Medical debt can have a profound impact on the quality of a person’s life. Studies have found that medical debt is associated with a decreased use of health services, especially among low-income individuals who often become sicker while delaying care, which increases the cost of their care (Crawford, 2021). These impacts can trickle down to affect the health of the entire community.
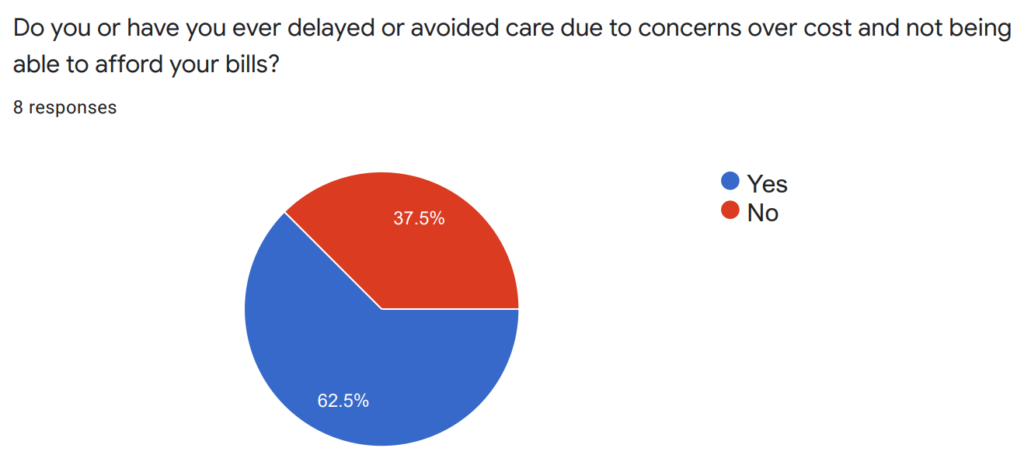
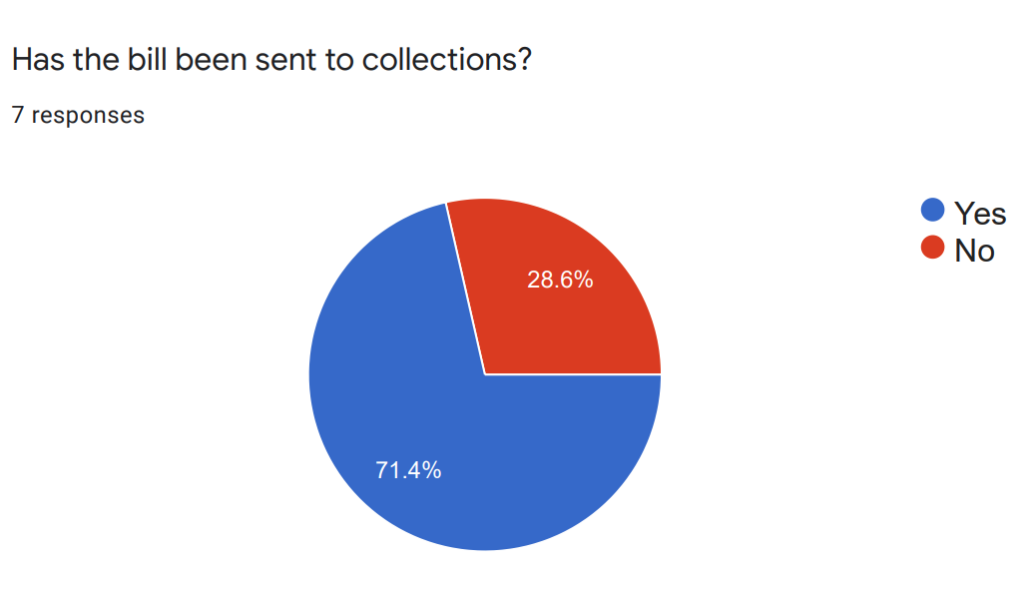
To better understand both the individual and community impacts of medical debt, Georgians for a Healthy Future, Georgia Watch, and SOWEGA Rising have used several outreach methods to invite residents of southwest Georgia to share their stories and feedback on experiences with medical debt. Since May of 2021, SOWEGA Rising has organized in-person listening sessions and Facebook Live virtual events to help individuals share their experiences with accessing and affording care in the community, including sharing whether they currently have unpaid medical bills, bills in collections, and how those bills are impacting their lives. So far, we’ve conducted seven listening sessions, and the experiences shared with us show that southwest Georgia residents are struggling to afford their care. Over 60% of those we spoke to reported delaying or avoiding care due to cost concerns, and over 70% reported an outstanding medical bill that had been sent to collections.
In October, we launched the Dish the Debt campaign in a focused effort to encourage community members, especially people of color who have been disproportionately impacted by medical debt, to share their encounters with medical bills, medical debt, and unfair debt collection practices. The campaign included social media posts throughout the month that talked about the issue of medical debt and explained why it’s so crucial for those affected by medical debt in southwest Georgia to share their story. Each post linked to a story collection form on Georgia Watch’s website where individuals could share their stories and contact information for follow-up.
A more recent effort to engage the southwest Georgia community to share their experiences with medical debt came during Georgians for a Healthy Future’s Southwest Georgia Health Care Affordability forum. During the forum, speakers from Albany Area Primary Care, Samaritan Clinic, and Valley Healthcare (local clinics that provide free or low-cost care to the community) shared how high medical costs negatively impact southwest Georgia. GHF also shared data on the disproportionate share of medical debt among communities of color in southwest Georgia during the forum. Each organization that spoke during the forum is also sharing links to the medical debt story collection form to elicit more stories from the southwest Georgia community.
Our organizations will continue to create opportunities for community feedback and stories regarding medical debt in southwest Georgia. We will ramp up our community feedback and story collection efforts in 2022, starting with a dual listening session and Affordable Care Act enrollment event in Cuthbert. We invite anyone interested to join us on January 13th, from 5 – 8 pm. Location in Cuthbert TBD.
We know that personal stories are critical to making lasting legislative and policy changes. While data on medical debt and the disproportionate impact on communities of color is deeply concerning, sharing stories creates a connection between those impacted by medical debt and Georgia’s decision-makers in a way that data cannot. We hope to use these stories, alongside data, to encourage hospital systems and lawmakers to enact policies that will protect Georgia communities from the crushing impacts of high health care costs and medical debt.
References
Crawford, K (2021). Stanford News: Stanford study finds medical debt is a double whammy for the poor. https://news.stanford.edu/2021/10/07/study-finds-medical-debt-double-whammy-poor/
Urban Institute (2020). Debt in America: An Interactive Map.https://apps.urban.org/features/debt-interactive-map/?type=overall&variable=pct_debt_collections

Georgia’s Medicaid health insurance system covers many different Georgians, including those with disabilities. The coverage provided to people with disabilities offers much-needed support to individuals and families that might otherwise fall short of addressing their health care needs.
While Medicaid has been a lifeline for some, a full expansion of Medicaid would bring additional funding to the state and strengthen existing programs. For every dollar Georgia would spend to close the coverage gap, Georgia would receive up to $9 in federal funding. The recently passed American Rescue Plan added to the financial incentives available under Medicaid expansion; under the new federal law, Georgia could attract $1.3-$2 Billion to cover the costs of expansion and offset state spending on other priorities.
This additional funding could benefit Georgians who need Home and Community-Based Services (HCBS) Medicaid waivers. HCBS waivers help people with disabilities get the health and support services they need so they can live independently in their communities, rather than in nursing homes or long-term care facilities. Currently, more than 6000 Georgians sit on a waiting list for one of these waivers. The additional funding that Georgia could earn under Medicaid expansion could reduce or possibly eliminate the HCBS waiver waiting list altogether.
Below is a first-hand account from a Georgia mother, whose 9-year-old daughter is covered by Medicaid. Her daughter was diagnosed with Ataxic Cerebral Palsy at 18 months. Since her diagnosis, the two have navigated challenging care and coverage issues. Their experiences highlight a number of the policy and advocacy issues that consumers contact GHF about regularly: Medicaid, Medicaid expansion, difficulty finding health care providers, Georgia’s public health system.
(more…)
GHF is excited to welcome Lois Hairston as the organization’s new Story Collection Coordinator. In this role, Lois will work to collect, develop, and share the stories of Georgia individuals and families as part of GHF’s Close the Gap initiative.
Lois is a graduate of Old Dominion in Virginia, where this past year, she served as the Communication and Membership Chair for the University’s Black Alumni Chapter. Her professional background includes experience with marketing agencies in Virginia and the District of Columbia, where she managed direct marketing campaigns for clients such as the Democratic Governors Association and the HealthWell Foundation. Recently, in her role as Communications Manager for Youth Entrepreneurs, Lois managed the creation of branded content and acted as the public relations liaison for the national nonprofit.
(more…)Recently released HHS numbers show that health insurance enrollment in Georgia and across the country is going strong. The Affordable Care Act is what has made these coverage gains possible, yet Congress has prioritized repealing this landmark legislation without clarifying what would replace it. We need your stories and your voice to ensure our policymakers understand the consequences of repealing the law. Please consider submitting your story, or the stories of the people that you serve, of how the ACA has benefited you. Whether it’s being able to afford coverage through the availability of tax credits, not being denied coverage due to a pre-existing condition, or being able to stay on a parent’s plan until age 26 – we need to hear from you!
numbers show that health insurance enrollment in Georgia and across the country is going strong. The Affordable Care Act is what has made these coverage gains possible, yet Congress has prioritized repealing this landmark legislation without clarifying what would replace it. We need your stories and your voice to ensure our policymakers understand the consequences of repealing the law. Please consider submitting your story, or the stories of the people that you serve, of how the ACA has benefited you. Whether it’s being able to afford coverage through the availability of tax credits, not being denied coverage due to a pre-existing condition, or being able to stay on a parent’s plan until age 26 – we need to hear from you!
Stay Connected
Archive
- April 2026
- March 2026
- February 2026
- January 2026
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- October 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- October 2023
- July 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- October 2022
- September 2022
- August 2022
- June 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- July 2014
- May 2014
- March 2014
- January 2014
- December 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- November 2012
- October 2012
- September 2012
- July 2012
- June 2012
- May 2012
- April 2012
- March 2012
- February 2012
- January 2012
- December 2011
- November 2011
- October 2011
- September 2011
- August 2011
- July 2011
- June 2011
- April 2011
- March 2011
- February 2011
- January 2011
- December 2010
- November 2010
- October 2010
- September 2010
- August 2010
- July 2010
- June 2010
- May 2010
- April 2010
- March 2010
- February 2010
- January 2010
- December 2009
- November 2009
- October 2009
